Corey Neu, University of Colorado Boulder
Sometimes cells can forget what type of cell they are and stop functioning correctly. This commonly happens in cancer, in which mature cells lose aspects of their identity and become more susceptible to begin dividing uncontrollably.
Heart conditions like cardiomyopathy, a disease that makes it harder to pump blood, affect the shape and function of affected heart cells. These changes can also occur in the nucleus of the cell, which houses genetic material that tells a cell how to function.
Because certain changes to nuclear structure can be early warning signals for heart problems, monitoring for such changes could help clinicians diagnose and treat disease before it gets worse. Researchers know that certain changes in the physical forces exerted on heart cells, including from their own contraction, can lead the cells to lose their heart cell identity and function poorly. But exactly how these physical forces work to change heart cell identity was unclear.
In a new study my colleagues and I published in the journal Nature Biomedical Engineering, we found that mechanical forces can reorganize the genetic material inside the nucleus of heart cells and affect how they develop and function. Better understanding of how cells claim and maintain their identities may help advance treatments to repair heart damage from cardiovascular disease and create new prosthetic tissues.
Pushing cell development in another direction
Early in human development, the external pressures surrounding immature cells influence what type of cell they eventually become when they differentiate, or fully mature. These external forces also help maintain tissue health as people age.
During differentiation, cells move around and restructure a mixture of proteins and DNA called chromatin that’s located in their nuclei. Cells use chromatin as a way to package and organize their genetic code. Knowing that external physical pressures can affect how cells mature, my research lab and I wanted to explore how mechanical forces can reorganize chromatin and what that might tell us about how heart cells develop and sometimes stop working.
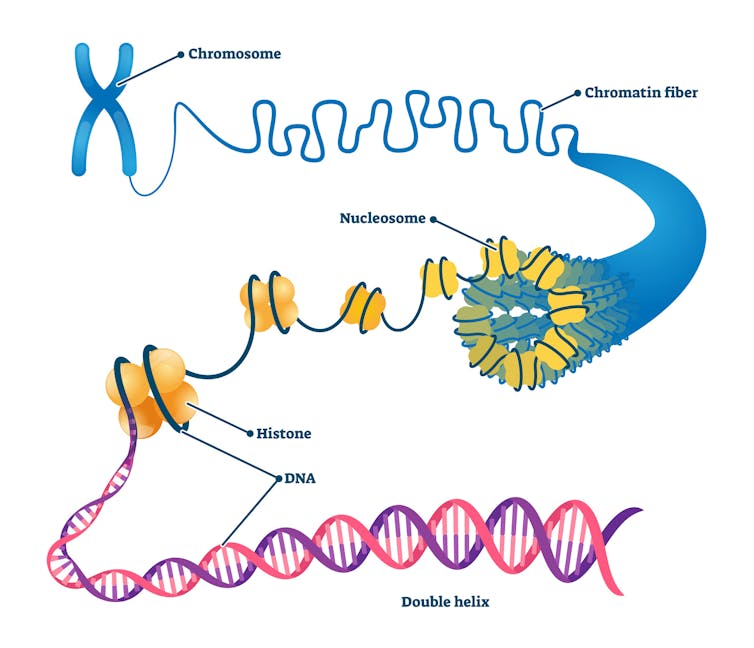
To do this, we looked at adult heart cells as they contracted under a microscope to see how their nuclei change shape. We then compared these images with the nuclei of embryonic heart cells as they normally change during early development. We found that areas in the nucleus with high tension tended to organize chromatin into specific shapes known to influence cell behavior. When we changed the tension in those areas of the nucleus, we were able to prevent cells from developing into normal heart cells. This meant that tension may play a key role in guiding heart cells on how to develop.
We then examined how mechanical stress changed the chromatin structure of heart cells from patients with cardiovascular disease and mice with reduced heart performance. Compared with healthy cells, heart cells from both patients and mice lost their chromatin organization and identity as heart cells. This meant that mechanical tension could influence how well mature cells function and their likelihood of developing into cardiovascular disease.
Mechanical forces matter in medicine
While our study explores the role that chromatic reorganization plays in early development, additional research is needed to understand exactly what triggers cells to develop into specific cell types. Further insight into how the mechanical environment surrounding a cell affects how it matures will help researchers better understand the process of human development.
[Over 140,000 readers rely on The Conversation’s newsletters to understand the world. Sign up today.]
Understanding what triggers a collection of cells to transition to a fully functional organ may also help researchers learn how to mimic these developmental processes and create new prosthetic devices. For example, accounting for the mechanical forces that affect how well tissue grafts for failing hearts and muscles work may help biomedical engineers design even more effective artificial implants. It may also set the stage for more organ-on-chip models that can be used instead of animals to screen potential drugs.
Corey Neu, Professor of Mechanical and Biomedical Engineering, University of Colorado Boulder
This article is republished from The Conversation under a Creative Commons license. Read the original article.