Anthony Jorm, University of Melbourne
Federal health minister Greg Hunt has unveiled a A$48.1 million COVID-19 mental health plan, featuring A$7.3 million for research and data collection, A$29.5 million for outreach to vulnerable people, and A$11.3 million for communication and other outreach programs.
This is on top of the A$1.1 billion Medicare package to tackle mental health and domestic violence, announced in March, which included funding for telehealth mental health services by GPs and mental health practitioners.
Is the funding needed?
Mental health experts have warned of a “second curve” of mental ill-health in the wake of the COVID-19 epidemic. This will result from widespread anxiety and depression, both about the disease itself and the knock-on social and economic effects of the lockdown.
Modelling has predicted that suicides could increase by 25-50% per year for up to five years, if urgent action is not taken.
It is hard to rely on any prediction with confidence, given this situation is unprecedented. Recent research from the Australian Bureau of Statistics indicates that the mental health effects of the pandemic are not dramatic so far. The graph below shows data from a national survey of symptoms carried out in April 2020, compared with earlier national survey data collected in 2017-18.
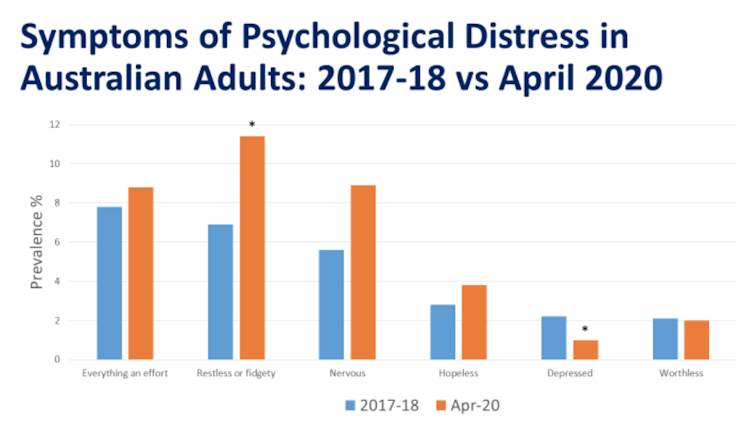
There has been a significant increase in feeling “restless or fidgety” and a trend towards more people feeling “nervous”. This probably reflects the confinement of the lockdown and anxiety about infection. Increases in anxiety are not necessarily a bad thing, as they motivate people to protect themselves against infection. Fortunately, the more serious symptoms of depression did not increase; in fact, there has been a signficant decrease in the number of people who report feeling “depressed”.
Similarly, early data indicate there has not been an increase in suicides in Australia, and Japan has actually reported a decline in suicides. This seems paradoxical, given the surge in unemployment and financial uncertainty.
Yet it has long been recognised that suicides can decrease during times of war if there is a greater sense of purpose and social cohesion. Whether our national response to the COVID-19 pandemic will also produce these protective effects is unclear, but the potential is there and should be encouraged.
While the early effects on mental ill-health have not been dire, it is very early days, and the predicted adverse consequences of the pandemic and lockdown may yet be seen. Given the uncertainties, the government’s planned investment in gathering better data seems wise.
Will it make a difference?
The biggest slice of the government’s new and previous funding packages will go towards extra Medicare services. But although this seems an obvious response, past experience indicates it is unlikely to have a major impact.
Over the past two decades, Australia has had hugely increased the provision of mental health services, but there has been no detectable improvement in the mental health of the population. One likely reason is that the extra services are not of sufficient quality to make a difference, with people not getting enough treatment, or services not being targeted to those most in need.
What seems more likely to have a beneficial effect is the funding put into the JobKeeper and JobSeeker schemes. The evidence is clear that mental ill-health is associated with job loss and low income. These schemes are keeping people in employment and providing incomes, which means they are directly tackling key risk factors for mental ill-health.
If this preventive benefit is to be maintained, it will be necessary to extend these schemes beyond the planned six months. Now that would be a real investment in the nation’s mental health.
Anthony Jorm, Professor emeritus, University of Melbourne
This article is republished from The Conversation under a Creative Commons license. Read the original article.












