Frances Darlington-Pollock, University of Liverpool; Ludi Simpson, University of Manchester, and Mark Green, University of Liverpool
For more than a century we have enjoyed sustained improvements to our life expectancy. Yet for the UK, there has been very little change in how long we can expect to live since 2011. And in England, the poorest have actually seen their life expectancy fall. To understand why this happened, we compared how the expected number of deaths differed from what actually occurred up to 2017-18, using official projections made in 2010 by the Office for National Statistics.
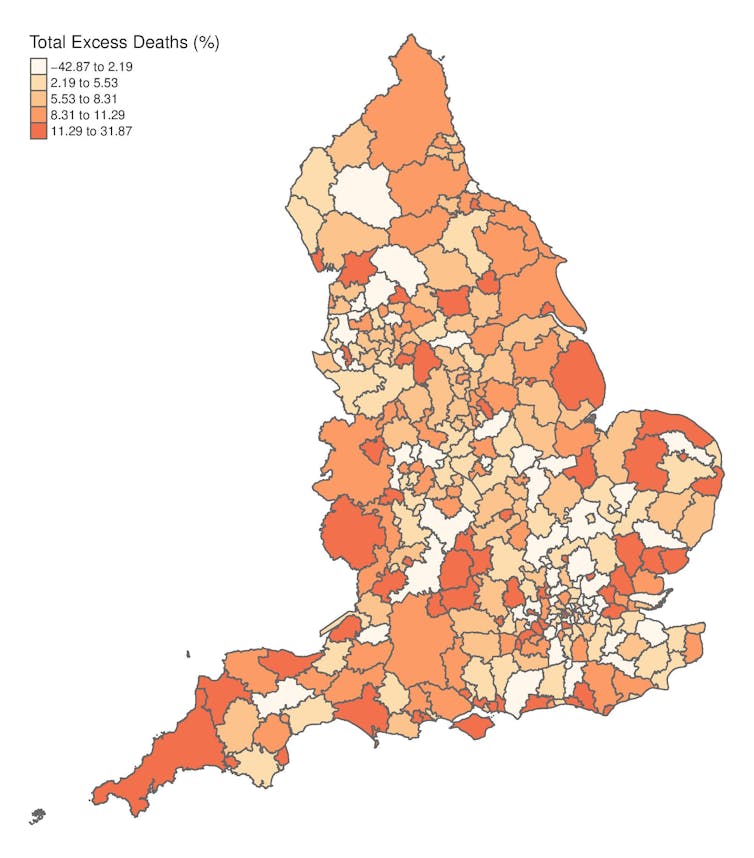
We estimate that 231,707 more people died between 2010-11 and 2017-18 than was originally anticipated. Over 90% of local authorities in England experienced more deaths than expected (see Figure 1). Almost 90% of these extra deaths have occurred since 2014-15, but well before COVID-19 struck.
This excess of deaths is striking because population projections tend to be conservative in their estimates of how life expectancy will change over time. They generally project a slower rate of improvement than is typically observed in reality. Projections are not cast with a crystal ball, and no demographer would expect to be spot on with numbers but estimates of more than 230,000 deaths than expected warrant investigation.
The austerity era
To pick apart what might explain the excess number of deaths, we tried to understand which areas had more excess deaths than others. Remarkably, levels of poverty or deprivation were not important. In other words, rather than finding more excess deaths in more deprived areas, there was no relationship between level of deprivation and number of excess deaths.
This is surprising because poorer communities have a disproportionate share of deaths for most, if not all, health conditions. It suggests that the issues behind the differences in excess deaths may be something that affects us all, irrespective of our social position. We must ask, then, why this population, at this point in time?
The period from 2010-2018 was characterised by a major policy shift. The introduction of fiscal austerity constrained local government spending and welfare provision. We found that in areas where welfare reforms led to a higher loss in average household income, excess deaths were larger.
We did not, however, find a similar relationship between excess deaths and deprivation. The impacts of austerity have been shown to be more keenly felt among poorer people and in more disadvantaged places. But it has also affected a wider range of demographics, from the so-called “struggling middle class” who have seen their pay fall over the decade of austerity to households with new parents who both work full time.
Though it would make sense to assume that older people would be disproportionately affected by these issues, that hasn’t been the case. In fact, excess deaths were most likely among working-age adults, while being the least likely among those aged 85+. This is largely because older age groups were able to enjoy the security of the triple lock protection for their pensions, buffering against the impact of wider welfare reforms at the time. No such protection existed for working age adults. Within this group, those more dependent on the security afforded by welfare provision would have of course found any cuts devastating.
Looking ahead
Our analyses do not prove that austerity caused 231,707 more people to die than should have. But evidence mounts about the harmful impacts of austerity on the health and wellbeing of the population. This plays out in different ways, such as through increasing unemployment or precarious employment, changes to benefits entitlements, and reductions to health and social care services. A return to fiscal austerity, as seen in chancellor Rishi Sunak’s stealthily austere budget or in future budgets, is likely to have significant implications for population health.
Though it may seem as though this sort of slow down is inevitable, the situation is more complex than it appears. It’s true that we don’t anticipate that life expectancy will increase indefinitely. And when we reach the limits of our longevity or indeed the limits of existing medical capacity, we will likely see a slowdown to improvements in life expectancy. But we are not at that point just yet. The UK already has a lower life expectancy than many other comparable countries, which means you’d expect us to continue improving, at least at the same rate that others are. And yet the opposite has been the case: we have seen even less improvement to life expectancy than other countries that have also seen a slowdown.
If England continues to underperform, we have to ask critical questions. Crucially, we’ll need to fully understand the context in which that underperformance plays out. This started long before COVID-19 took hold. So if prime minister Boris Johnson is really committed to “doubling down on levelling up”, “building back better” also has to mean building back different.
Frances Darlington-Pollock, Lecturer in Population Geography, University of Liverpool; Ludi Simpson, , University of Manchester, and Mark Green, Senior Lecturer in Health Geography, University of Liverpool
This article is republished from The Conversation under a Creative Commons license. Read the original article.












