Andrea Pattinson, University of Sydney and Amanda Salis, University of Western Australia
It’s true a number of the health conditions which we know increase the risk of severe illness from COVID-19 are also associated with obesity. These include type 2 diabetes, high blood pressure, heart disease and respiratory disease.
But new research suggests obesity independently is a strong predictor of severe illness, particularly in those aged under 60 years.
This is concerning given two-thirds (67%) of the Australian adult population have a body mass index (BMI) in the overweight or obese range.
BMI is a person’s weight in kilograms divided by the square of their height in metres (kg/m²). While it’s an imperfect measure for an individual person, BMI is very useful in comparing health and weight across a population and between groups.

For adults, overweight is a BMI of 25 or above, but less than 30kg/m². For a woman of average height (162 cm), this would be equivalent to a weight of 66kg or above, and for a man of average height (176 cm), a weight of 78kg or above.
Obesity is defined as a BMI of 30kg/m² or above. This equates to a weight of 79kg and above for a woman and 93kg and above for a man, both of average height.
The evidence
One study from China looking at data from 112 patients reported overweight and obesity were almost five times more prevalent in patients with COVID-19 who died (88%) compared to those who survived (19%).
Preliminary data from another Chinese study involving 383 patients, although not yet peer reviewed, suggests overweight or obesity more than doubled the risk of developing severe pneumonia as a result COVID-19, particularly in men.
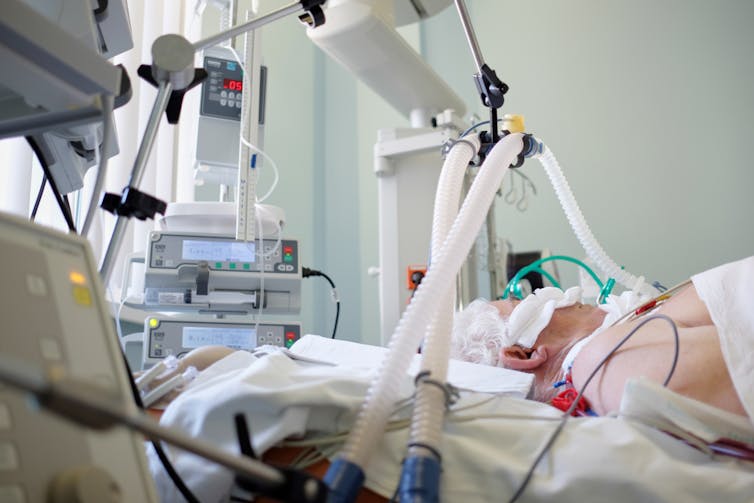
Researchers in France found almost half of 124 patients admitted to an intensive care unit (ICU) with COVID-19 had a BMI in the obese range. This was nearly double the rate of a comparison group of ICU patients with severe acute respiratory disease unrelated to COVID-19.
Further, the need for mechanical ventilation increased with increasing BMI.
A UK surveillance study of patients admitted to intensive care with COVID-19 reported almost three-quarters (75%) of the 6,720 patients had a BMI in the overweight or obese range, which is greater than the population prevalence of overweight and obesity in adults in the UK (around 67%).
Although some of these studies factored in chronic conditions when reporting their results, it’s difficult to separate all of the conditions associated with obesity that may contribute to some degree to the poorer outcomes.
So it’s likely that some – but not all – of the increased risk of severe COVID-19 associated with obesity could be due to people having other chronic conditions.
Young people
It seems obesity may have more of an impact on the severity of COVID-19 in young people, according to two studies from New York.
One study of 3,615 people who tested positive for COVID-19 found those aged under 60 years with a BMI of between 30 and 34 were almost twice as likely to be admitted to ICU compared to patients with a BMI of less than 30. This likelihood increased to 3.6 times in those patients with a BMI of 35 or greater.
In patients over 60 years, the researchers didn’t find a significant link between obesity and severe illness (as indicated by admission to ICU).
Another study, which recorded weight for 178 patients, found obesity was the most common underlying condition for patients aged under 64 years admitted to hospital for COVID-19.
Why the greater risk?
Taken together, the above data suggest there is an association between obesity and more severe COVID-19 illness, particularly in those with a BMI of 35 or greater.
The US Centers for Disease Control and Prevention (CDC) now lists “severe obesity” as a risk factor for serious COVID-19 illness.
We don’t know exactly what role obesity plays in the severity of COVID-19 symptoms. But the mechanisms are likely to be multifaceted, particularly since obesity itself is the result of a complex interaction between genetic, hormonal, behavioural, social and environmental factors.
We know obesity can have a significant impact on lung function. Excess weight around the abdomen can compress the chest, making it more difficult for the diaphragm to move and the lungs to expand and take in air. This can contribute to lower levels of oxygen in the blood, which may exacerbate the symptoms of COVID-19.
We also know obesity results in a chronic state of inflammation which can impair the body’s immune response. This could potentially make it more difficult for the body to fight coronavirus.
The challenges in caring for patients with severe obesity may also affect their outcomes from COVID-19.
For example, it’s more difficult to intubate or perform imaging such as X-rays and CT scans in patients with obesity.
Further, positioning ventilated patients on their stomachs can increase the amount of oxygen entering the lungs. But this is often not possible for patients with severe obesity.
Should I be worried?
The short answer is no. If your body weight is above the healthy range, these results should not be cause for panic or impetus to engage in crash diets to reduce COVID-19 risk.
While the data does suggest obesity is a risk factor for more severe illness, it’s early days in the life of COVID-19 and we need more research before we can definitively say what’s going on.
The most significant thing you can do to lower your risk is to follow the government’s guidelines.

These restrictions can be challenging and might lead to reduced physical activity and eating for comfort or to ease boredom, potentially resulting in weight gain.
If you find yourself with extra time during the pandemic, you may find it helpful to view it as an opportunity to make healthy choices and cultivate new habits to reduce your risk of illness in general and to enhance health and well-being going forward.
Andrea Pattinson, PhD Candidate, University of Sydney and Amanda Salis, NHMRC Senior Research Fellow in the School of Human Sciences, University of Western Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.












